Are you experiencing pain in your back or neck that’s worse when sitting or standing? If so, it’s possible that you may be suffering from a degenerative disc disease. In this article, we’ll explore the various symptoms of this condition and how to get relief from the debilitating pain. Let’s dive in and discover if degenerative disc disease is the cause of your discomfort!
Contents
Why Do Discs Degenerate?
Degenerative disc disease (DDD) is a common cause of chronic low back and neck pain. This condition occurs when the discs located between the vertebrae (bones in the spine) start to deteriorate due to everyday wear and tear. DDD can be caused by a variety of factors, including age, injury, lifestyle choices, and genetics.
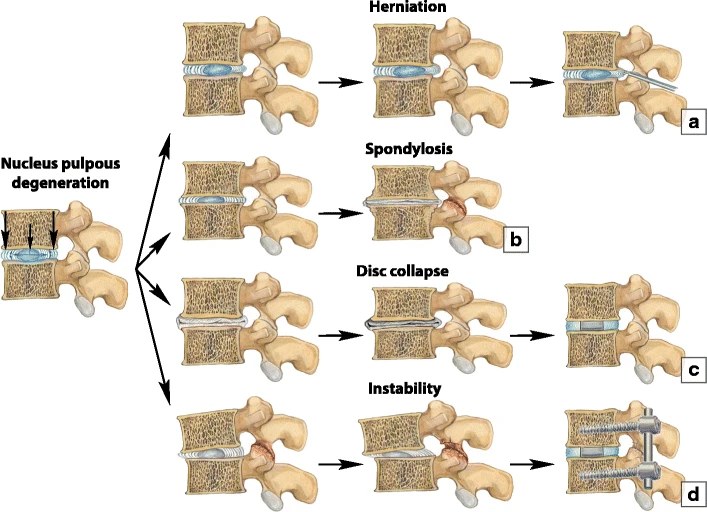
As individuals get older, their discs naturally lose moisture and flexibility making them less able to resist everyday movements which results in small stress tears in the outer wall of their discs. This can cause the vertebrae bones they sit between to move closer together resulting in little shock absorption.
Due to intervertebral discs not being able to perform shock absorbing duties as they used to anymore, it means that our spine is not subjected to less cushioning as we age, making us more susceptible to damage from everyday activities. If untreated, water content within these intervertebral discs also decreases leaving them more brittle and less responsive which also increases your chance for injury due to overstretching or jarring motions which are necessary for our everyday lives such as bending forward or running upstairs.
Signs Of Degenerative Disc Disease
Degenerative disc disease refers to a condition in which the discs, which act as cushions between your vertebrae, become damaged and are unable to provide enough support. This can cause chronic pain and other issues, including loss of mobility and nerve damage. If left untreated, it can become increasingly severe and lead to further health complications.
The signs of the condition vary depending on how advanced it is but some common symptoms are:
- Persistent pain in the lower back that may radiate down one or both legs
- Stiffness or reduced range of motion in the back and/or neck
- Numbness or weakness in arms, legs, hands, or feet due to impaired nerve signals from compressed nerves
- Muscle spasms, often accompanied by tightness in the lower back area due to inflammation
- Uneven posture due to weakened muscles around the spine and ribs
- Difficulty standing for too long or participating in activities like running due to discomfort from movement
If you have any of these symptoms that don’t go away with rest or medications, then it’s likely you may be suffering from the early stages of degenerative disc disease. It’s important that you visit a doctor right away so they can diagnose you properly and get proper treatment before it becomes worse.
Neck Pain
Neck pain is a common symptom of degenerative disc disease. Degenerative disc disease usually results when the discs between your spinal vertebrae become worn down over time. As this happens, the cushioning properties of the discs decrease, which in turn can lead to chronic neck pain.
In severe cases, when degenerative disc disease has progressed beyond a certain point, it can result in nerve damage and even spinal stenosis (a very serious condition where too much space is created between two or more vertebrae).
Patients with degenerative disc disease might also experience bladder and/or bowel control issues due to nerve damage resulting from the narrowed space between the discs in their spine.
This occurs when pressure builds up on sensitive nerves that are no longer protected by tissue and becomes worse as more of these nerves become compressed. It is important to talk to your doctor if you start to experience any of these symptoms so they can diagnose and treat them properly.
Numbness and Tingling
Degenerative disc disease can cause a variety of symptoms, such as numbness and tingle in extremities due to nerve compression or irritation. Numbness is defined as the partial or complete loss of sensation. Tingling is defined as an abnormal spontaneous prickly or irritating sensation, often likened to feeling like pins and needles.
Numbness and tingling can be triggered by degenerative disc disease (DDD) when the pressure on the nerve root is enough to affect the sensation in some way. People may experience numbness, burning, or a pins-and-needles type of sensation in their arm and leg depending on which nerve root is affected by the disorder.
These sensations can range from mild to severe, depending on the extent of damage to their nearby discs in the spine. Some people may also experience similarly surprising muscle weakness in addition to any numbness or tingling they are experiencing due to DDD.
Other common symptoms that have been linked with DDD include pain at night when lying down, localized backache related to certain activities during the day, and generalized pain from standing upright for too long – all of which could potentially be coming from pinched nerves due to DDD pressure on them.
If these sensations become too uncomfortable for an individual then it’s important that they seek medical advice immediately so that any further complications can be avoided.
Traveling Pain
Traveling pain is one of the most common symptoms of degenerative disc disease (DDD) and is a symptom that often surprises patients. This type of pain manifests itself in other locations, making it difficult to diagnose and treat. DDD occurs when the discs in your spine become worn down and unable to cushion the vertebrae as effectively as before, resulting in shooting pains traveling to various parts of the body.
When suffering from DDD, you may experience pain due to the pressure on other areas of your body that are compensating for changes in the spine. Pain can occur suddenly without warning or build up gradually over time depending on how active you are going about activities that impact the spine: bending, stretching, or lifting incorrect weights may create additional strain on already weakened discs and exacerbate your symptoms.
The discomfort created by DDD may affect different parts of your body including your neck, shoulders, arms, and even legs depending upon where discs have been affected by wear and tear. This kind of discomfort can be aggravated through everyday activity such as sitting for long periods at a desk or standing for long periods at work and could even trouble you while trying to sleep during night hours.
Your doctor may suggest physical therapy if these pains become chronic so learn how to prevent exacerbations to your condition if possible through correct posture techniques, custom-tailored exercise regimes, and lifestyle changes where they might apply.
Pain That Improves When You Change Activities
Pain that improves when you change activities may be one of the primary symptoms of degenerative disc disease. Disc pain is caused by destructive processes taking place in the spinal discs between vertebrae. Discs are fluid-filled structures with a central core of large, round cells and outer fibrous layers that allow for a small amount of movement in the spine. When this process occurs, it’s called disc degeneration.
When the outer layers of a spinal disc become weak or even tear, it causes structural damage and destabilization which can cause considerable pain. The pain can either radiate along the length of the spine or be localized to an area around the disc itself.
Pain that improves when you change your activity is strongly indicative of spinal degeneration as some activities will put less strain on affected discs than others do. For example, sitting up straight might make someone with a degenerating spinal disc feel much better than if they were standing upright or kneeling down. Additionally, certain motion exercises that consciously flex and move different vertebrae may also reduce pain in those areas due to decreased pressure on affected discs.
It’s important to note that this type of symptom does not always mean nerve root compression has occurred; it’s merely indicative of underlying damage to one or more discs in the spine region which can still occur without additional medical intervention since nerve roots were left unaffected by injury or tear in exterior layers only
Worsening Pain After Switching Positions
When you are dealing with degenerative disc disease (DDD), it’s important to be aware of how your changing body position can impact the severity and frequency of your symptoms. Worsening pain after switching positions is one of the most common signs that degenerative discs are causing discomfort.
The discs that cushion your spine from the force of your body weight and pressure throughout everyday activities like sitting, standing, walking, or bending can degrade over time. When this occurs, the disc becomes less able to absorb physical shock or movement and is weakened. As a result, moving your body or shifting positions causes these already-damaged discs to compress further leading to an increase in pain.
Discs that have been damaged by DDD will mostly feel worse while you’re in certain positions including sitting for long periods of time, arching your back too far backward, slouching when seated, or laying on one side for too long. You might also start to notice signs of worsening degenerative discs when you bend forward excessively either quickly or repeatedly, take part in activities such as heavy lifting, pushing objects overhead, and leaning too far in any direction.
Often times muscle spasms occur as well when worsening pain is being caused by DDD due to the inflamed muscles trying to protect the spine from increased pressure from misalignment caused by weak discs.
Immediate relief from DDD-related pain can be found through stretching exercises and moderate levels of physical activity as well as cooling treatments like ice packs and anti-inflammatory medications recommended by your doctor. Once these methods reduce irritation for temporary relief though it’s important to follow up with an assessment from a spinal specialist who can accurately diagnose the root cause in order to find a long-term treatment plan that works best for you.
Pronounced Pain In Your Lower Body
Degenerative disc disease can cause pronounced pain in your lower body, notably in your lower back. This form of pain can begin suddenly or may develop over a period of time. You may experience mild or sharp pains running from your lower back down through the affected area in your legs. These sensations can often be a sign of a herniated disc, where the cushion between two discs is weakened and impinges upon the nerve roots connected to it.
The effects of degenerative disc disease often include persistent pain resulting from the wearing down or bulging out of spinal discs due to age-related degeneration. This condition tends to worsen with time due to increased pressure on any one disc as well as loss of flexibility in that particular part of the spine.
Symptoms may also range from mild aches and pains to severe issues depending on severity and location, such as sciatica where you get shooting pain that runs southward through one leg when pressure is put on the sciatic nerve.
It’s important to schedule an appointment with a doctor if you experience any signs and symptoms that could be linked with degenerative disc disease since timely diagnosis ensures that treatment is effective at managing discomfort and restoring activity levels as soon as possible. Moreover, nerve damage needs prompt attention in order for minimal risk complications to occur.
Treatment Options
Degenerative disc disease is a condition affecting the discs that stress or control movement between the vertebrae in your spine. Treatment for this disorder is typically conservative and noninvasive, beginning with lifestyle changes such as smoking cessation and weight loss if needed. These modifications can help to reduce the pain associated with DDD and any other issues that may have contributed to its development.
Physical therapy is also recommended for anyone suffering from DDD as engaging in regular exercising can help promote the strengthening of the back muscles. Steroid injections are sometimes used for the relief of inflammation and pain, but should usually be avoided due to potential side effects. Additionally, lumbar braces have been known to provide short-term relief but don’t address the root cause of disc degeneration.
More sophisticated treatments are available too, such as ablation treatment using heat energy or undergoing radiofrequency ablation (RFA). Both treatments aim at gently eliminating some of the painful disc material without completely disrupting its structure while providing significant symptom relief.
In certain cases, facet injections are also used to treat pain coming from surrounding bony structures instead of focusing on disc damage while maintaining motion preservation.
Finally, more minimally invasive treatments include artificial annular disruption (AAD), endoscopic discectomy, nucleoplasty, and X-STOP Interspinous process device implantation. Although these methods carry a risk of complications, they have helped many people regain their active lifestyle free from chronic pains caused by degenerative disc diseases over time.
Conclusion
In conclusion, degenerative disc disease is a very common spine condition that can be effectively treated in most cases. Treatment options depend on the severity of the condition, but typically involve lifestyle modifications, physical and occupational therapy, or a combination of these approaches.
More severe cases may require spinal fusion, joint injections, or artificial disc replacement surgery. However, it is best to discuss all available options with a spine specialist before making any decisions.
It is important to recognize the signs and symptoms of degenerative disc disease early. If it is suspected that you are suffering from this condition, seek medical advice from your healthcare provider as soon as possible to ensure proper treatment and reduce further damage to your spine.
Avoiding alcohol consumption and creating ergonomic workstations can also help alleviate pain and discomfort associated with Degenerative Disc Disease. For more information on Degenerative Disc Disease please contact an experienced spine surgeon or your healthcare provider for diagnosis and treatment options.

Alan Walker is an author, researcher, and contributing writer at Spine Institute NY. He is a typical introvert, coffee fanatic, and freelancer.”

